Latest News

LATEST NEWS
Our next Principal: Alyson King
Published 12th March 2026

LATEST NEWS
Reasons to Apply to Brasenose College…
Published 13th February 2026

LATEST NEWS
Professor Sir Mike Stratton wins Jessie Stevenson Kovalenko Medal
Published 30th January 2026
Professor Sir Mike Stratton, an honorary fellow at Brasenose College, has been awarded the 2026 Jessie Stevenson Kovalenko Medal by the National Academy of Sciences of the USA, which is the equivalent of the Royal Society.

LATEST NEWS
Student Blog: A Community Like No Other!
Published 6th January 2026
I thought I was dreaming. My parents were in tears, but I was absolutely ecstatic when I moved into Brasenose.

LATEST NEWS
Brasenose alumnus David Szalay wins the Booker Prize 2025
Published 11th November 2025
Huge congratulations to Brasenose alumnus David Szalay (English, 1992) who has won the Booker Prize 2025 with his novel Flesh.

LATEST NEWS
Study blog: A summer on Skomer Island
Published 11th November 2025
Over the summer, two Brasenose biology students spent time on Skomer Island in West Wales doing Fieldwork. Here’s their student blog on their summer.

LATEST NEWS
Brasenose Organ restoration shortlisted for the Oxford Preservation Trust Awards
Published 10th November 2025
We are delighted to announce that the Brasenose Organ restoration has been shortlisted for the Oxford Preservation Trust Awards.
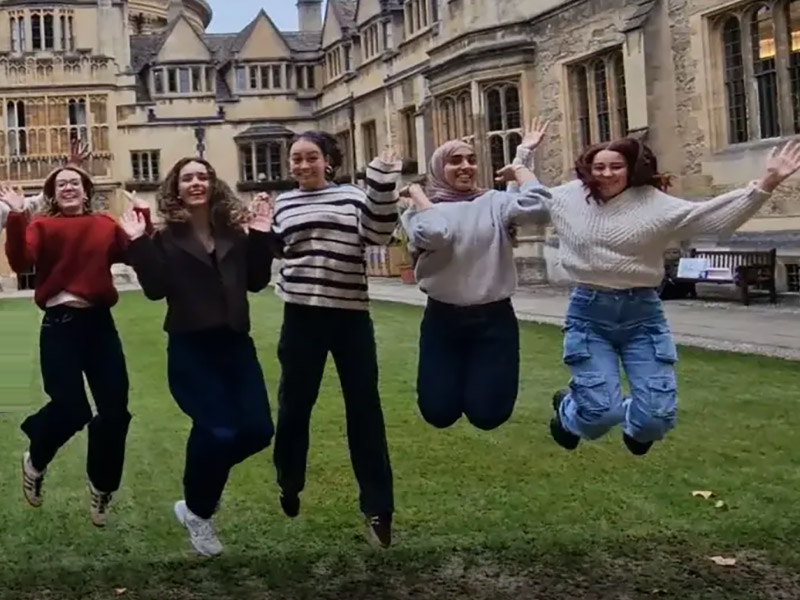
LATEST NEWS
Brasenose Giving Day 2025
Published 9th November 2025
Giving Day is coming on 13 and 14 November, which means getting the chance to celebrate what it means to be a part of Brasenose.

LATEST NEWS
The Mercy Step
Published 10th October 2025
Former Brasenose student Marcia Hutchinson has published her first novel, The Mercy Step.

LATEST NEWS
Exploring Lithuania: The new Grigas Award for Brasenose students
Published 9th October 2025
Brasenose College is delighted to announce the creation of the Grigas Award
LATEST NEWS
Professor Richard Robson - Nobel Prize Winner
Published 8th October 2025
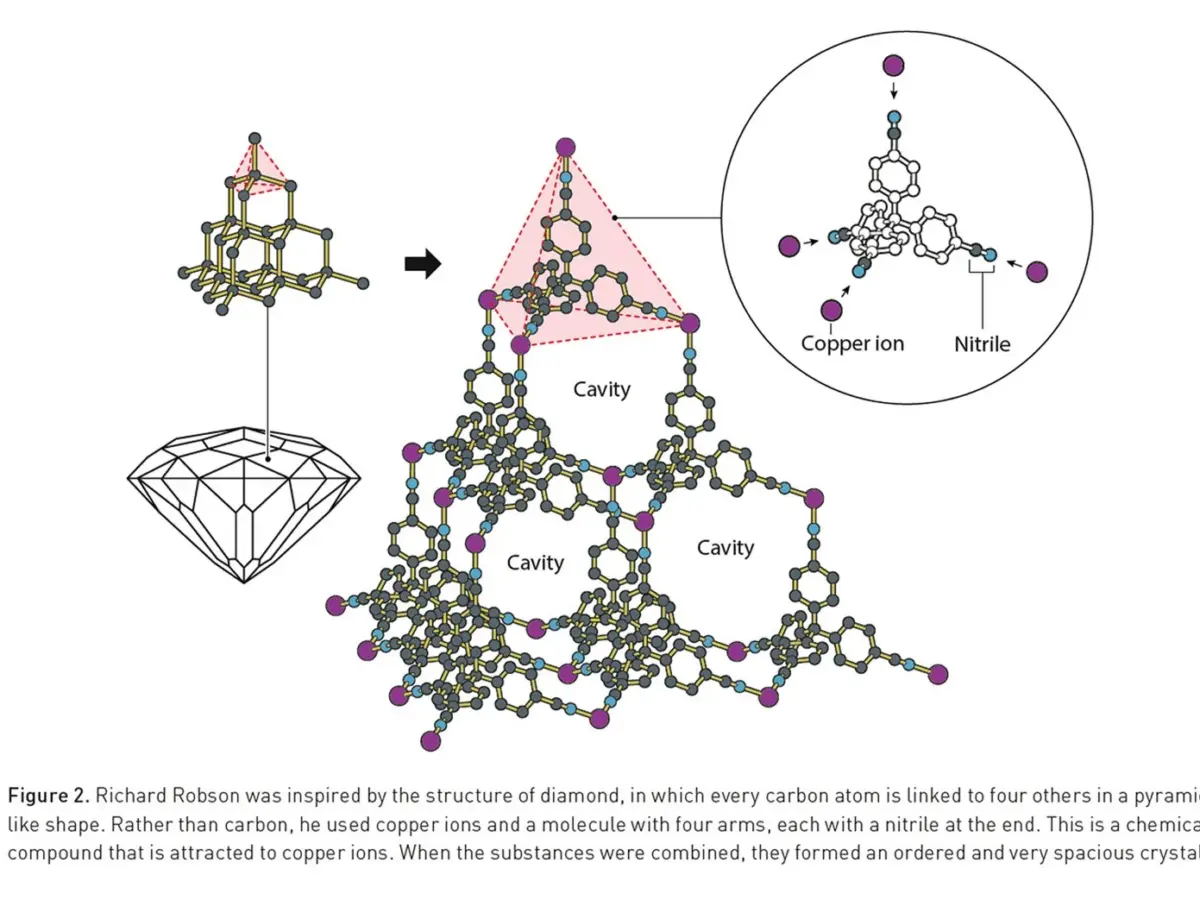
The Brasenose community is proud to offer its congratulations to alumnus Professor Richard Robson (Chemistry, 1955) on being awarded the Nobel Prize in Chemistry for 2025, along with Susumu Kitagawa and Omar Yaghi “for the development of metal-organic frameworks”.
Image: ©Johan Jarnestad/The Royal Swedish Academy of Sciences

LATEST NEWS
Luna Memorial Travel Fund
Published 7th October 2025
The Luna Memorial Travel Fund has been established in loving memory of Luna